About Tay-Sachs Disease

What is Tay-Sachs Disease?
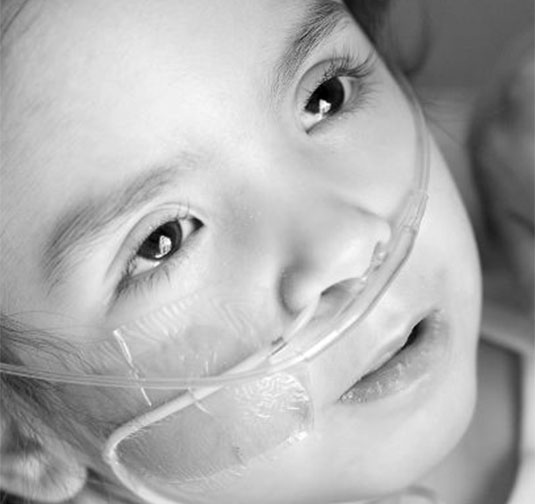
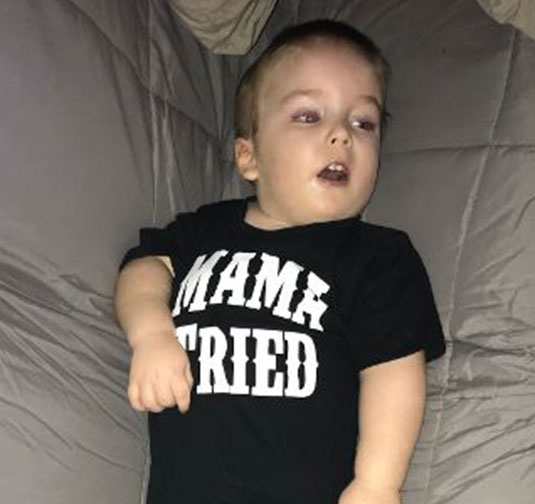
Tay-Sachs disease (TSD) is a hereditary condition caused by mutations in the Hex-A gene, leading to a deficiency or absence of the Hex-A enzyme. This deficiency causes fatty waste products to accumulate in cells, particularly nerve cells in the brain, causing cell swelling and death. The Hex-A gene was identified in 1985 and since then, roughly 75 to 100 mutations linked to TSD have been discovered.
TSD manifests in Infantile, Juvenile, or Late On-Set forms. Both Infantile and Juvenile forms are untreatable and fatal, while the Late On-Set form progresses slower but remains devastating. Disease progression correlates with Hex-A levels; Infantile cases, often devoid of Hex-A, progress rapidly, typically resulting in death by age 3. Symptoms, undetectable at birth, reveal themselves months later. TSD can affect families with no prior history of the disease. Carriers can be identified through enzyme assays or DNA studies of blood samples, which measure Hex-A levels. The National Tay-Sachs & Allied Diseases Association (NTSAD) offers a list of certified screening locations. As there is no cure, genetic testing in high-risk groups and prenatal testing for affected fetuses are crucial
The 3 Levels of Tay-Sachs Disease
Tay-Sachs disease manifests in three different onset stages. The stage of onset is typically established by medical practitioners based on the age at which the person first started showing signs of the disease.
Infantile
Symptoms typically appear between the ages of 3–6 months of age.
Juvenile
Symptoms typically appear between the ages of 2–5 years of age.
Late Onset
Symptoms typically appear in adolescence and into adulthood.